
Best Onco Gynecology Hospital in Mumbai
A cancer diagnosis changes everything — sometimes in an instant. The questions come fast, and finding the right answers, from the right people, matters more than almost anything else at that point. At OMA Hospital, we’ve built our onco-gynecology department with exactly that in mind.
Gynecologic oncology in Mumbai has come a long way — and we’re proud to be part of that progress. Our team doesn’t just treat cancer. They sit with patients, explain what’s happening, help them weigh their options, and stay with them through treatment and beyond. That’s not a promise we make lightly.

What you’ll find here is a team that understands the female reproductive system in its entirety — because our specialists also work across gynecology and fertility care. That joined-up perspective changes how we approach onco-gynecology, especially for younger women where preserving fertility remains part of the conversation.

Most people are familiar with the word ‘oncology’, but onco-gynecology is a more specific branch — and one that doesn’t get nearly enough public attention.
Onco-gynecology is the medical specialty that focuses on cancers originating in the female reproductive system. That includes the cervix, uterus, ovaries, vagina, vulva and fallopian tubes. It’s a field that sits at the intersection of cancer medicine and women’s health — and it requires specialists who understand both deeply, not just one or the other.
In India, the numbers around gynaecological cancers are hard to ignore. Cervical cancer alone remains one of the leading cancer-related causes of death among women. Ovarian cancer is frequently diagnosed late because early symptoms are vague and easily dismissed. Uterine cancer cases are rising alongside shifts in lifestyle and hormonal patterns. These aren’t just statistics — they’re women who, in many cases, could have had very different outcomes with earlier detection and specialist care.
At OMA, our approach to gynecologic oncology in Mumbai is built on three things: early detection, personalised treatment, and genuine human support throughout the process. Treatment plans are shaped by the type and stage of cancer, yes — but also by who the patient is, what her life looks like, and what matters most to her.
Concerned about a symptom or a recent result? Don’t sit with it alone.
Types of Cancers Treated at Our Hospital
Our specialists are experienced across the full range of gynaecological cancers. Here’s what we treat — and a little about what each one involves:
Cervical Cancer
One of the most preventable cancers when caught early. Routine screening through Pap smears and HPV testing — available as part of our diagnostic services — can detect abnormal cell changes long before they become cancerous. For women already diagnosed, our team offers surgical, radiation and chemotherapy options depending on the stage.
Ovarian Cancer:
Often called a ‘silent’ cancer because the early symptoms — bloating, mild pelvic discomfort, changes in digestion — are easy to attribute to other things. By the time many women are diagnosed, the cancer has already spread. This makes specialist-led surveillance genuinely important, particularly for women with a family history or known genetic mutations like BRCA1 or BRCA2.
Uterine (Endometrial) Cancer
The most common gynaecological cancer in developed countries, and increasingly common in India. It often presents with abnormal uterine bleeding — which means women who report this symptom promptly actually have a real advantage. Caught early, the prognosis is generally very good. Our team manages both surgical and adjuvant treatment approaches.
IUI (Intrauterine Insemination):Vulvar Cancer
Less common, but important to diagnose correctly. Vulvar cancer can be mistaken for skin conditions or infections for months before a biopsy is performed. We see patients who’ve been going around in circles elsewhere — and getting a clear diagnosis, even a difficult one, is the first step toward doing something about it.
Vaginal Cancer
Rare but serious. Vaginal cancer is often picked up during routine gynaecological examinations or as a secondary finding during investigation for another concern. Multidisciplinary management — surgery, radiation or a combination — is typically involved.
Fallopian Tube Cancer
One of the rarest gynaecological cancers, and historically one of the most difficult to diagnose prior to surgery. The symptoms overlap significantly with ovarian cancer, and management is similarly complex. Our team’s experience across both conditions means patients aren’t passed between departments when the picture isn’t immediately clear.
Gestational Trophoblastic Disease (GTD)
A group of rare tumours that arise from the tissue that forms the placenta. GTD sits uniquely at the intersection of oncology and maternity care — it occurs in association with pregnancy, which makes it both emotionally complex and medically specific. Our team’s combined expertise in both areas is particularly valuable here.
Diagnostic & Screening Services at OMA Hospital
The difference between catching something early and catching it late can be the difference between a straightforward procedure and a much harder road. We take screening seriously — not as a checkbox, but as a genuine line of defence.
Pap Smears and HPV Testing:
The most effective screening tools for cervical cancer. A Pap smear takes minutes. An HPV test adds another layer of information. Together, they can identify abnormal changes years before cancer develops. Accessible through our gynecology department as part of a routine well-woman visit.

Colposcopy:
When a Pap smear returns an abnormal result, a colposcopy lets us examine the cervix more closely. It’s a short, outpatient procedure — not painful, but important for determining whether further intervention is needed.
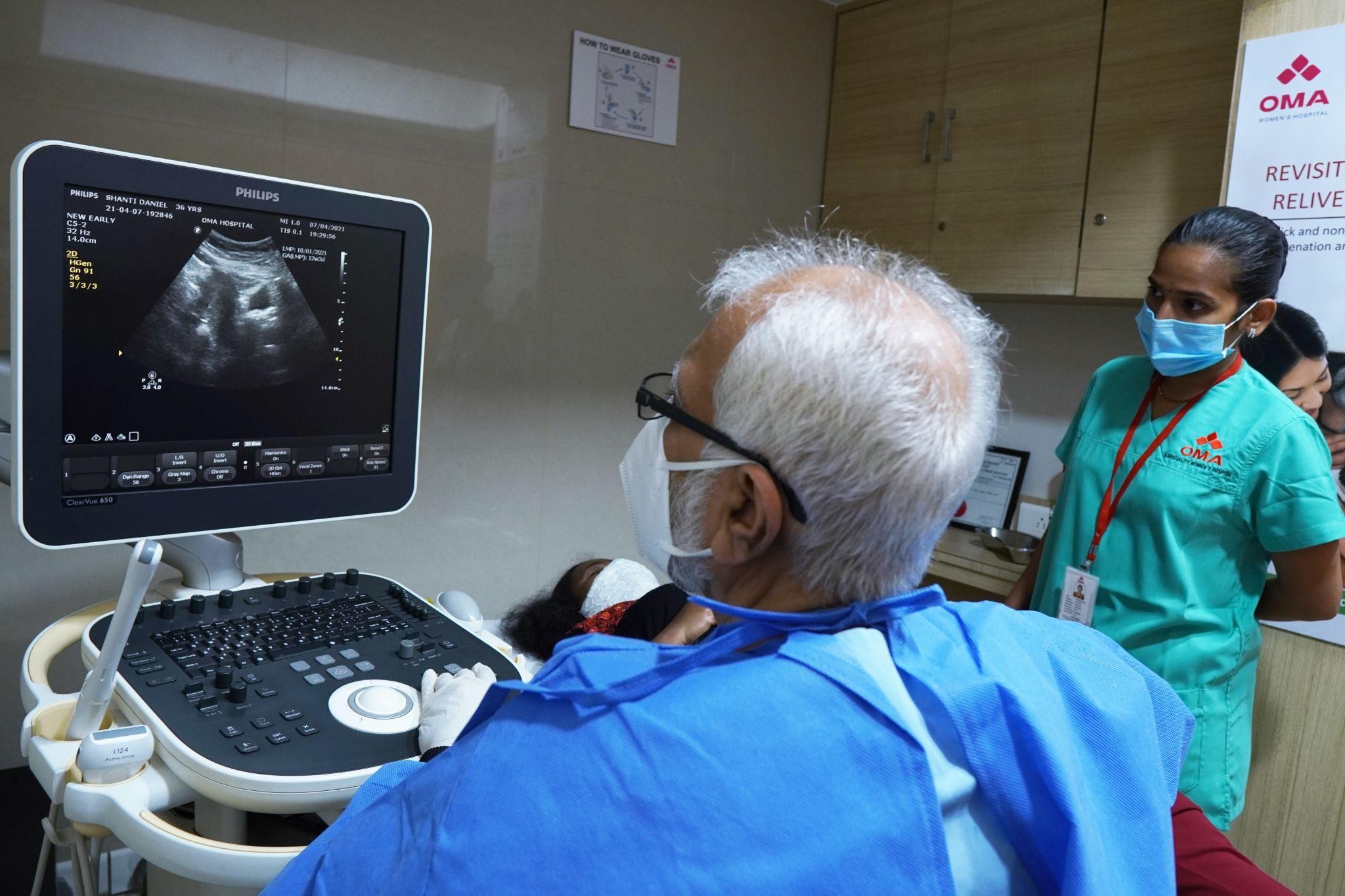
Imaging — Ultrasound, CT and MRI:
Our radiology team performs pelvic ultrasounds, CT scans and MRI imaging to assess the extent of disease, check lymph nodes and guide surgical planning. Having this capability in-house means results are discussed quickly and next steps are decided without delay.
Endometrial Biopsy:
For women with abnormal uterine bleeding, an endometrial biopsy provides tissue samples for analysis. It’s a key diagnostic step for ruling in or out uterine cancer, and it’s done as a clinic procedure in most cases.
CA-125 and Other Tumour Marker Tests:
Blood tests that measure certain proteins associated with ovarian and other gynaecological cancers. Not diagnostic on their own, but used alongside imaging and clinical findings to build a fuller picture.
Diagnostic Laparoscopy:
When imaging isn’t conclusive, a minimally invasive surgical approach allows our team to directly visualise the pelvic organs and take biopsies where needed. Often the fastest route to a definitive answer.
Genetic Counselling and BRCA Testing:
For women with a significant family history of breast or ovarian cancer, genetic counselling and BRCA1/BRCA2 testing can clarify personal risk and shape prevention strategies. This is offered alongside our broader fertility preservation discussions for younger women who are not yet ready to have children.
Second Opinion Services:
If you’ve received a diagnosis elsewhere and want it reviewed by our specialists before deciding on a treatment path — that is entirely something we support. It’s not starting over; it’s making sure you’re informed.
Want to know more about screening or get a second opinion?
Treatment finishing is not the same as care finishing. This is something we feel strongly about at OMA, and it shapes how we structure follow-up for every patient who’s been through onco-gynecology treatment here.
Recovery from gynaecological cancer treatment — whether that’s surgery, chemotherapy, radiation, or a combination — affects the body and the mind in ways that don’t resolve the moment active treatment ends. Fatigue, hormonal changes, physical recovery from surgery, emotional processing — all of it takes time, and all of it deserves attention.

Structured Follow-Up Consultations:
Regular post-treatment reviews are scheduled from the outset — not as an afterthought. These appointments exist to monitor for recurrence, manage any lasting side effects, and make sure the transition back to everyday life is supported properly.
Physiotherapy and Pelvic Floor Rehabilitation:
Surgery and radiation in the pelvic region can affect bladder, bowel and sexual function. Our team works alongside physiotherapy support and our gynecology specialists to address these concerns directly — not dismiss them as ‘expected side effects’.
Hormonal Support and Menopause Management:
Treatments like surgical removal of the ovaries or certain chemotherapy protocols can bring on early menopause. We address the symptoms — hot flushes, bone density changes, mood shifts — and discuss hormone therapy where it’s appropriate and safe given the cancer type.
Psychological and Emotional Support:
A cancer diagnosis and its treatment leave a mark that isn’t always visible. Anxiety, depression, fear of recurrence — these are real, and they deserve proper support. We connect patients with counselling as part of the care journey, not as a separate, optional service. Our patient resources also include guidance on emotional wellbeing during and after cancer treatment.
Nutritional Counselling:
What you eat during and after cancer treatment genuinely matters — for energy, healing, immune function and managing treatment side effects. Our nutritional guidance is practical and tailored, not a generic printed sheet handed out at discharge.
Fertility Preservation Discussions Post-Treatment:
For younger women who wish to explore family options after treatment, conversations about fertility don’t end at diagnosis. Our IVF and fertility team works closely with the onco-gynecology department to explore what’s possible — whether that’s embryo freezing before treatment or other options afterwards.
Palliative Care Integration:
For patients with advanced or recurrent disease, palliative care is about quality of life — managing pain, controlling symptoms, and supporting both the patient and their family through a difficult period. This care runs alongside treatment, not instead of it.
Long-Term Survivorship Care:
Women who complete treatment and enter remission still need monitoring — for recurrence, for the long-term effects of treatment, and for any new health concerns that arise. We don’t discharge and disappear. Survivorship follow-up is a real, structured part of what we offer.
Why Choose OMA Hospital as the Best Onco-Gynecology Hospital in Mumbai?
There are several hospitals in Mumbai with oncology departments. What makes OMA specifically worth considering for gynecologic oncology in Mumbai is the combination of specialist depth, integrated care and the way patients are actually treated from first appointment to last follow-up.


Specialists with Genuine Depth in Women’s Cancer:
Tanuja Uchil (MBBS, DGO, DNB – OB-GYN, MNAMS) leads a team whose expertise spans gynaecology, oncology and fertility. This isn’t a general oncology department that also sees gynaecological patients — it’s a team built specifically around women’s cancer care.



Full Spectrum of Treatment Under One Roof:
Surgery, chemotherapy, targeted therapy, immunotherapy, radiation coordination, palliative care, psychological support, nutritional counselling, physiotherapy and fertility preservation — it’s all available here. Patients don’t have to stitch together a care team from multiple hospitals.
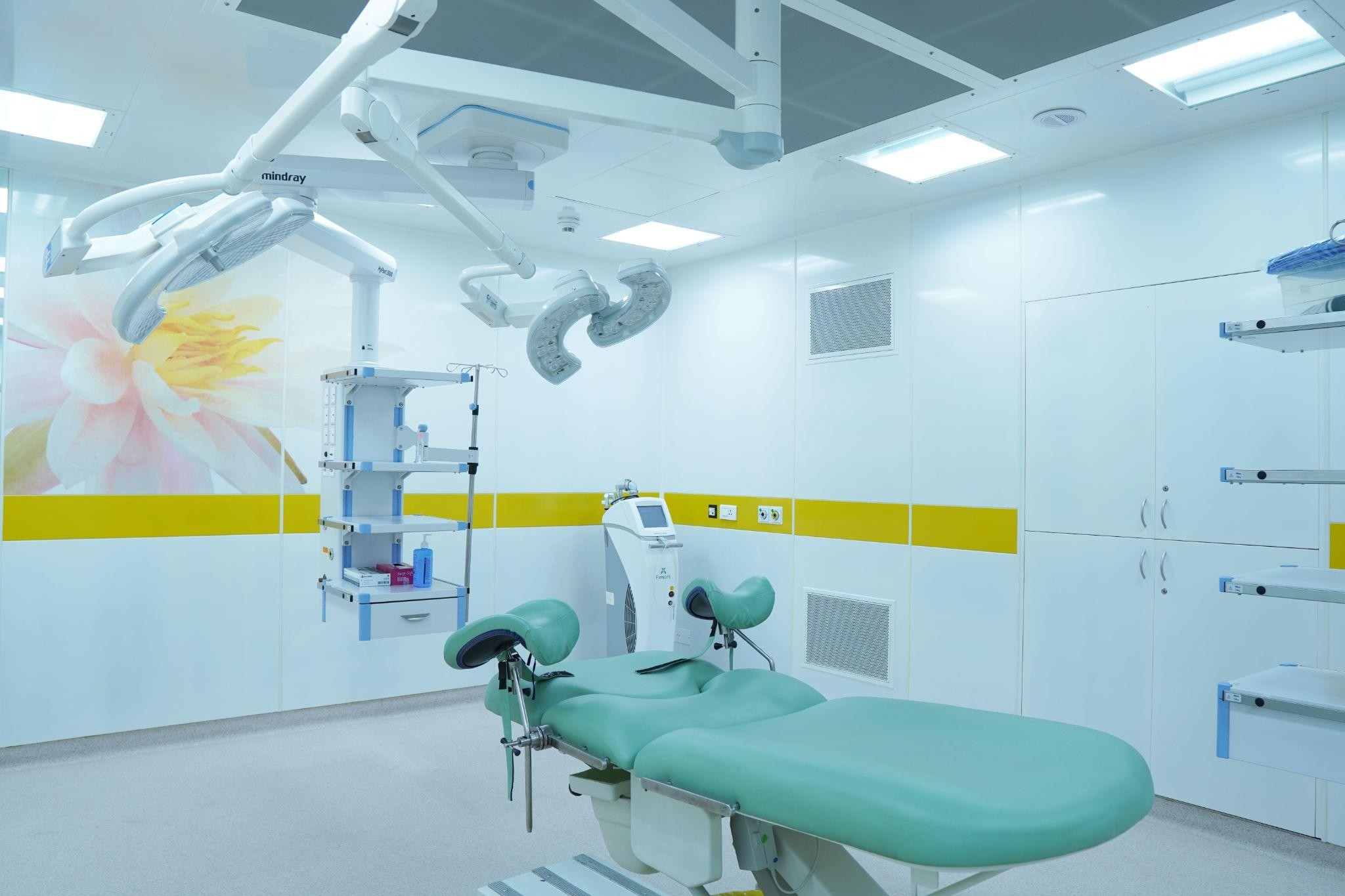
Certified Class 10000 Clean Room Operating Theatres:
Our surgical OTs meet internationally verified standards for sterility and infection control. Stainless steel walls, advanced air circulation systems, OT lights from Steris (France), surgical tables from Maquet (Germany), anaesthesia systems from Belgium — the infrastructure matches the clinical ambition.
Integrated with Radiology for Fast Results:
Having our radiology and diagnostics team on-site means imaging results come back quickly, MDT discussions happen without waiting weeks for external reports, and treatment planning moves at the pace the patient’s situation demands.
Fertility Awareness Built Into Cancer Care:
For women who are diagnosed before completing their family, this matters enormously. The link between our onco-gynecology and IVF and fertility teams means fertility preservation conversations happen as part of the treatment planning process, not as a separate referral that falls through the gap.
Connected to the Full OMA Women’s Care Ecosystem:
Beyond onco-gynecology, OMA offers maternity care, aesthetic and regenerative gynecology and more. For patients who need care across multiple specialties — which is common in cancer treatment — being in one place matters.
Honest Conversations, Always:
We tell patients what they need to know. About prognosis, about treatment side effects, about what the realistic options are at each stage. That honesty isn’t always easy to deliver, but it’s always respectful — and patients deserve it.
Accessible from Across Mumbai:
Located at Chembur East, OMA is well connected from most areas of Mumbai. During treatment, when fatigue is real and travel adds up, that matters more than people often expect when choosing a hospital.
FAQs
What is an onco-gynecology hospital?
An onco-gynecology hospital specializes in diagnosing and treating cancers of the female reproductive system, including ovarian, cervical, uterine, vaginal, and vulvar cancers.
When should I consult an onco-gynecologist?
You should consult a specialist if you experience symptoms like abnormal vaginal bleeding, persistent pelvic pain, unusual discharge, or have a family history of gynecological cancers.
What types of cancers are treated at an onco-gynecology hospital in Mumbai?
Common cancers treated include cervical cancer, ovarian cancer, uterine (endometrial) cancer, vaginal cancer, and vulvar cancer.
Are gynecological cancers curable?
Many gynecological cancers are treatable and even curable, especially when detected early. Treatment success depends on the type, stage, and overall health of the patient.
What treatments are available for gynecological cancers?
Treatment options may include surgery, chemotherapy, radiation therapy, targeted therapy, and immunotherapy, depending on the condition.

